Racial Justice is a Matter of Life and Death
The protests taking place across the country are calling on all Americans to recognize, discuss and address hard truths about racial injustice in the US. So is the demographic data that has emerged from the COVID-19 pandemic. Given the longstanding inequities in income, housing and criminal justice faced by Black, Indigenous, and People of Color in the US, it might have been predicted that they would be more vulnerable to the COVID-19 pandemic. But the size of the race gaps in COVID-19 mortality is shocking. Current CDC data shows the age-adjusted death rate for Black people is 3.6 times that of white people, and the death rate for Hispanic/Latino people is 2.5 times that of white people. The gaps are biggest among working-age people: Among those aged 35-44, for example, Blacks are 10 times more likely to die of COVID-19 than whites, and Hispanic/Latino people 8 times more likely.
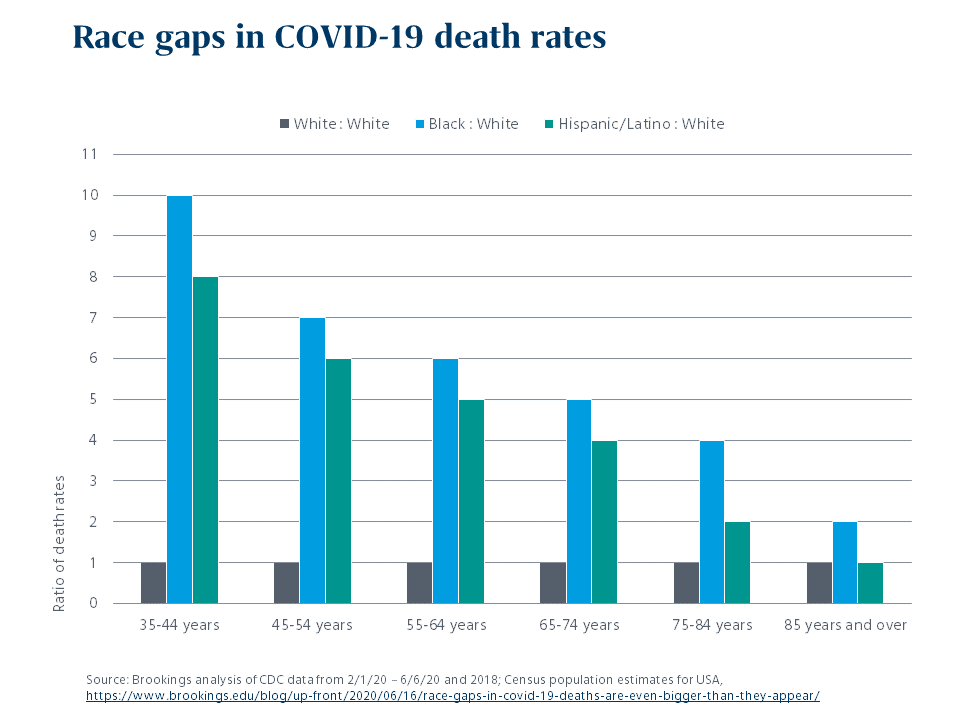
Greater exposure to the virus is certainly a factor. Blacks and other people of color disproportionately perform the essential jobs that can’t be done remotely; they also have less ability to socially distance at home and in their communities. In addition, once infected, they have worse outcomes both because of greater prevalence of underlying health conditions such as hypertension, obesity, diabetes, and lung disease, and because they have less access to health care.
Employers looking to optimize the health and well-being of workers and their families need to understand that that the pandemic is exposing, in the harshest possible light, disparities in health and health outcomes that have long existed. Just as the video of George Floyd’s killing has made it impossible not to see the catastrophic reality of racism, the clearly unequal effects of the pandemic call on us to educate ourselves about the impact of racism on health and to work to change it.
Many employers have already rejected the notion that good health is equally available to anyone willing to practice good health habits, and some have begun to invest in initiatives that address the social determinants of health (the conditions in which people are born, live, and work). This is important work, which must continue and should be accelerated. But our efforts need to acknowledge a disturbing truth: That beyond the disparities in income, housing, and social support, there is evidence that simply experiencing racism in everyday encounters also has serious health consequences for Black people. Dr. David R. Williams, a sociologist at the Harvard School of Public Health, has spent 20 years studying this subject and is the lead author of an enlightening paper published last year. I watched his TEDMED Talk, which he begins with the story of a Yale-educated Black man who died at age 62 in the midst of a life of professional success and family happiness. He goes on to reveal that early deaths were typical for the other Black graduates of the class of 1970; 41 years after leaving Yale, their mortality rate was three times the average of their classmates. This story illustrates what his research has proven: That structural racism, cultural racism and individual-level discrimination – even for those with more education and opportunity – takes a harsh physical toll.
What actions can employers take to counter the racism that erodes the health and well-being of Blacks and other people of color? It’s critically important that leadership acknowledge the problem and communicate a plan of action. But we are all responsible for bringing about change. A thoughtful Black colleague sent me a link to a panel discussion called "Equipping White Women to Speak Up Against Racism" – three Black women and three white women working in corporations who were willing to have uncomfortable, invaluable conversations about race. The message came through loud and clear: We need to listen, we need to educate ourselves, we need to acknowledge that systemic racism exists. And we need to start changing what each of us can change, now.
